Glocal health Consultants
"Glocal support on glocal issues –
health policy and implementation thought leadership"
The nature of the silent arrow
Let’s start at the end
Let’s tell the story of health. And let us start at the end, because that – for reasons that will become apparent in the remainder of my argument – is how we do things in academia. ‘How we do things in academia’ is unspoken and intrinsic to curriculum design and implementation (and the tools we maintain to keep things as they are – rather than shake them up) and funding our research.
Recently I have started work with CHETRE – the Centre for Health Equity Training Research and Evaluation. It is a dream job, because the Centre does what I have been arguing for many years: bring together research, policy and practice by intentionally blurring the boundaries between the three, and explicitly taking a scholarly activist stance. CHETRE is part of the University of New South Wales, and of the South-Western Sydney Local Health District (for those of you not in Australia: ‘Local’ is the land mass of a small European country; ‘Health District’ means exactly that: all actions, appreciations and interventions in the full chain of health development and restoration, from working with local governments on urban planning and housing policy and practice, to high-tech health care operations in operating theatres). We have dual appointments in both institutions.
I did something in my first hundred days at the CHETRE Director that I think very few academics do. Politicians, yes. Maybe the occasional government bureaucrat, OK. And perhaps, on the off-chance, business entrepreneurs because they need to know the people that should buy their products (but then, usually, those folk contract some expensive consultants to do focus groups and some internet research). What I did was walk around in the neighborhoods that should benefit of CHETRE’s work, and talk – to the street-level bureaucrats and to the community developers. But I also listened… Sat down to have a coffee and tried to gauge what concerns people – particularly about their health of course.
And I realized there was very little in my arsenal of academic rhetoric, my toolbox, that resonated with the stories I heard. My fancy toolbox of political theory, of concept and network mapping, and of arguing why addressing the social, commercial and political determinants of health is the only sensible way toward a healthier and more equitable society.
So let’s tell the story from the end – because that is what we do, and what we teach our students.
The causes of health – a whirlpool of conjecture
In 1853 Thomas Wakley, the first editor of The Lancet, complained: “…all is darkness and confusion, vague theory, and a vain speculation. Is it a fungus, an insect, a miasm, an electrical disturbance, a deficiency of ozone, a morbid off-scouring from the intestinal canal? We know nothing; we are at sea in a whirlpool of conjecture.” (The Lancet II, 1853, p. 393) He was talking about the origins of cholera, but could have been writing about the vast majority of 19th century health challenges. These days, however, the dominant health services delivery paradigm no longer embraces ideas of balance in the cosmos, the Hand of God, the equilibrium between hot, cold, wet and dry, or invisible miasma that would challenge our health. No, in the modern, allopathic, biomedical world model nearly all problems have been solved. Disease is caused by pathogenic agents (viruses, bacteria, toxins, prions) or simply by wear and tear (e.g., arthrosis, deep vein thrombosis, some would say diabetes). The few remaining mysteries should be resolved soon – in the biomedical disease care model. This paradigm remains important in maintaining the force and dominance of what has been called the medical-industrial complex.
On the fringe of, and just outside this complex we find an ever-growing network of health (not disease) researchers that have wondered what causes health and well-being. A popular model was developed by Whitehead and Dahlgren at the invitation of the European office of the World Health Organization in the 1980s – used and referenced on the internet nearly 50,000 times.

It is an appealing rainbow of proximal and distal factors impacting on individual and community health. The appeal may be due to an apparent simplicity what causes health: there are things beyond us that influence our health, and those things are shaped by yet other things. But I would claim that virtually no-one that is referring to the work by Margaret and Göran actually has read the original report or its edited WHO version, and appreciates the conceptual strength and policy relevance – even 25 years after its initial rise to prominence.
Another way of looking at the causes of health was found in a bunch of Canadians’ journey trying to explain why some people are healthy and others not. They intended to dig really deep into the biomedical explanation and looked for stress response differentials between people from higher socio-economic strata (SES) and lower ones. They surmised that higher SES groups have learnt do deal with stress better than lower SES groups – learning through intergenerational evolutionary development, but also (intergenerational) life-course learning and immediate stress response learning – which would explain how the social gradient impacts on health opportunity. But even Evans, Barer and Marmor, editors of this book, needed to acknowledge that all of this stress response stuff is exacerbated by many other factors – which they neatly describe, and then suggest how systems interventions actually would facilitate people across the social gradient to respond to unhealthful situations more resiliently and equitably.
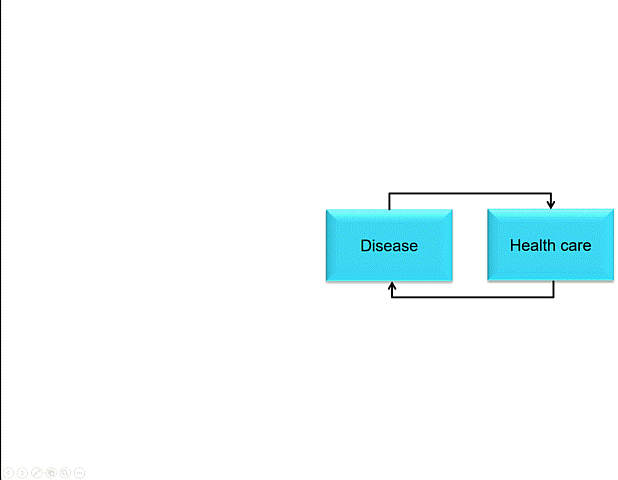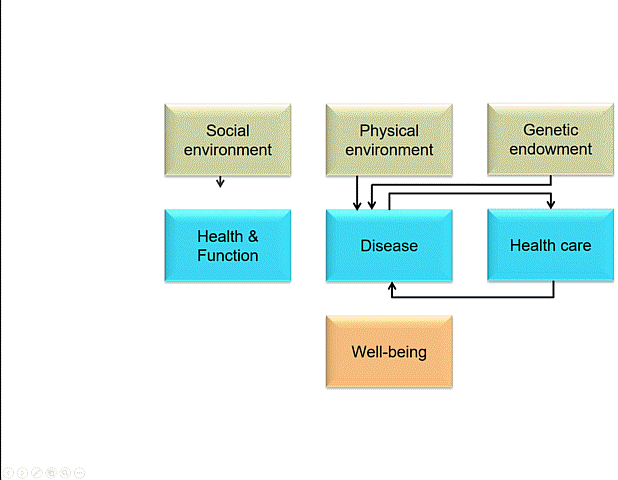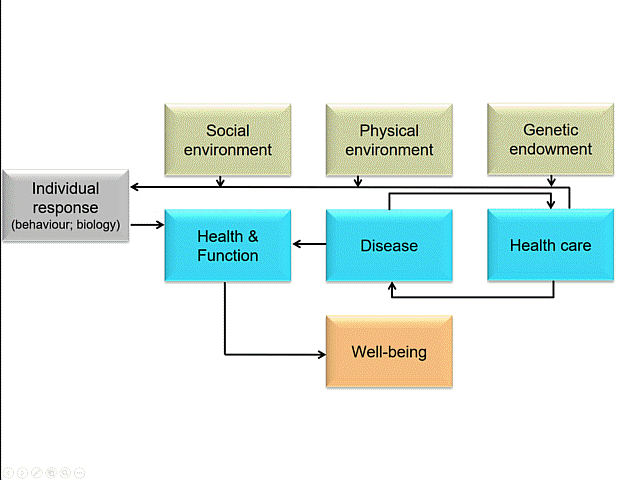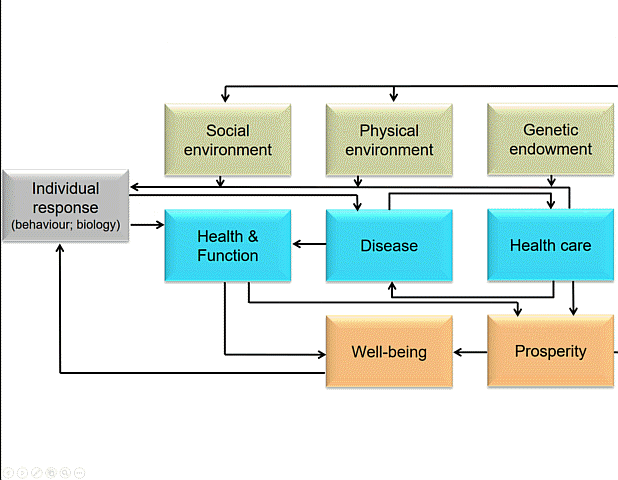
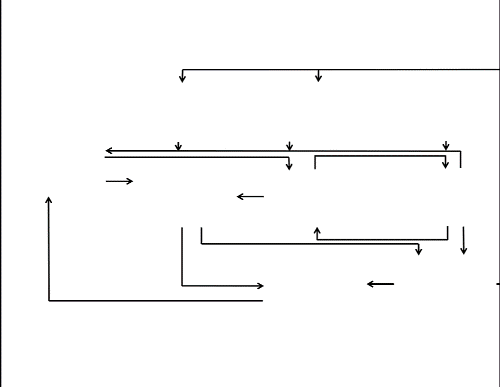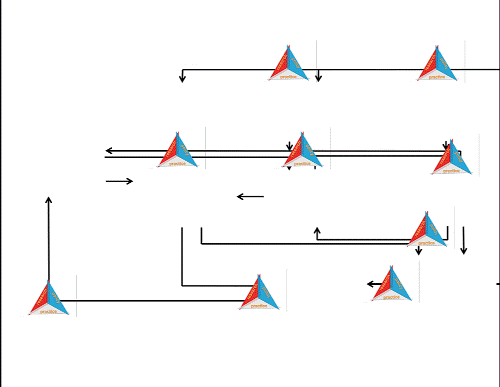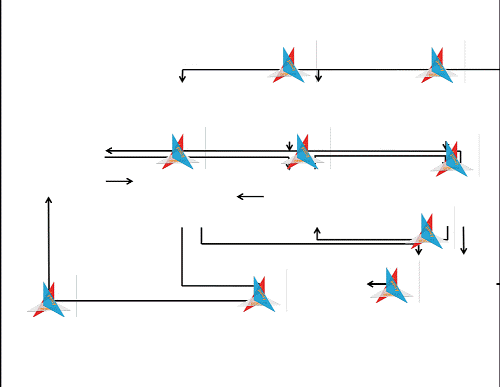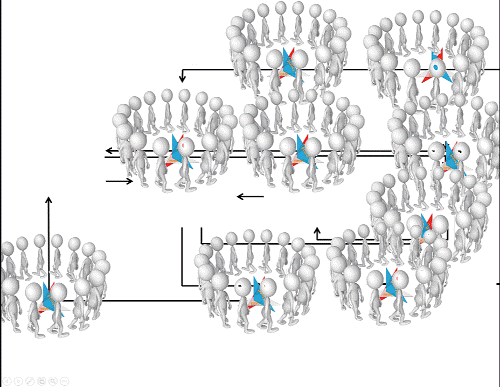
I like this model. Not because it makes more sense than Whitehead and Dahlgren’s, but because it does something else. It has a whole bunch of arrows.
The arrows and the action
Arrows are important visual tools. They imply causality, or at least some kind of relationship, with the arrowhead pointing the ‘right way’. I would suggest that apart from suggesting causality (a relationship between cause and effect) arrows can also indicate finality (a relationship between intervention and outcome) and normative hierarchy (something can be considered superior to, or in control of, something else). Many constructs in the scholarly world, I think, would benefit from more hygienic thinking about such relations. Arrows, for their linkage connotations, are important because we can challenge their direction, strength, and even presence; they are not necessarily ‘natural’. In the ‘Why are some people healthy’ model the arrows, I surmise, are the places where we should intervene. The arrows designate the spaces in our social construction of the world where we could unleash policy, organisational change, administrative protocol and challenge or build on existing practice. The arrows are the places where action at the nexus between research, policy and practice is necessary and would yield impact that matters.
But wait – arrows are also the places where people are. Where they live, love, work and play. Where they make, for instance, the relationship between well-being and prosperity happen. Arrows are about community.
‘Community’ has not been a neglected element in the public health and health promotion discourses. A Google Scholar search for ‘community’ and ‘health’ in titles since the year 2000 yields approximately 22,400 ‘hits’ (with nearly 80,000 since indexing by Google started). Also, we do see a slow but steady increase in focus from the scholarly rhetorical to a scholarly empirical perspective.
In the social determinants of health discourse, arguments to involve ‘community’ have been pervasive. Blas and colleagues even see its role as absolutely essential. They appeal to an understanding of community as an environment or situation that can mobilise its potential – in connection and coordination with other influential actors – to change the (determinants) world around them. The potential is there. Is it in fact mobilised?
There are reviews how communities actually take control of their (economic, social, and health) destiny. For instance, Jagosh and colleagues demonstrate that community-based participatory research yields better and more sustainable health efforts and outcomes. Others review how partnering in the community between a range of government and non-government actors effectively contributes to health improvement. But these excellent reviews at best peripherally touch on community action for policy development, leaving alone holding public administration accountable to (or change it to better address) the complexities of social determinants of health and health equity. Fortunately, strong evidence is emerging (particularly sponsored by the World Bank for mostly non-OECD countries) that certain forms of community decision-making are effective: deliberative and participatory decision-making allocates resources better, for greater (health) equity.
The literature is, however, rife with cautions to see community participation as the miracle solution to dealing with complexity in a network age. Crawshaw, Bunton and Gillen have analysed appeals to community action as a means of reinventing the relationship between the individual and society, and the championing of civic responsibility. To achieve this, neo-liberal ideology frames the role of individuals as active citizens with both rights and responsibilities, and with a duty to participate. Thus, community is promoted as a panacea for reconstructing civil society, a middle ground between statist models of ‘society’ and market models of the ‘individual’, both of which are understood to have failed as modes of governance. This reinvention of community as a site of social and political action has been influential in both policy and academic discourses, as shown by the emergence of ‘new’ concepts such as social capital and capacity building.
But does the community ‘get’ health?
Consistently, opinion polls around the world show that ‘health’ is one of the highest valued attributes of individuals and communities. One would expect that, with such high priority, people are willing to act on ‘health’.
One investigation sought to review systematically the impact of community engagement on health. The authors found only 13 studies with methods rigorous enough to be included (but found strong suggestions that community engagement ‘works’). Interestingly, the notion that communities determine their destiny by influencing policy, and civil and public institutions is not captured in the conceptual heuristic that underpins the study. Why? The work by Commers may shed some light on this question. It maps the understanding of the Dutch population, media and politicians of social determinants of health and finds that unprompted queries such as ‘what is health?’ and ‘what determines your health?’ produce responses that neatly fit with the biomedical paradigm. In other words: the Dutch community prioritises proximal determinants of health (pathogens and lifestyles) over more distal determinants (such as corporate interests, politics, systems parameters). Commers also finds that, if prompted appropriately (for instance, by asking ‘who determines your health?’), the same community quite adequately frames virtually all social determinants of health as important.
Australian researchers find that the connection between community concerns, activism and the public health professional world is troubled. They investigated lay understandings of (the causes of) health inequity. The authors conclude that “… the findings in this study are evocative of a kind of collective inertia within the public health field. The lack of congruence between explanations and public policy responses suggests that public health arguments directed at addressing the social determinants of health have not become absorbed into bodies of lay knowledge.” Clearly very few communities, or members in communities, ‘get’ social determinants well enough to start advocating for it at a systems level, be it through participatory budgeting, through influencing policy processes, or through activism aimed at reshaping public administration.
One of very few research efforts to consider what it would take to mobilise communities politically towards a more substantive social determinants policy effort has been undertaken by the Robert Wood Johnson Foundation. Over four years they systematically investigated frames and metaphors for health in the United States and found that there is a meaningful divide between language and rhetoric deployed by public health professionals and scholars, and what the US public (across the Democratic-Republican spectrum) feels. The social determinants message needs to resonate at a deep metaphorical level – which obviously is culturally determined and as contextual as the social gradient itself.

I have argued that, perhaps, in our quest for understanding health and the causes of health inequity, we have retreated too much into the ivory towers – or silos – of academia and public health professionalism. We have created a language and complex diagrams that may not ring true to the lived experience out there.
And so we come to the beginning
It wouldn’t be unwise, no it is imperative, to remind ourselves that we do not want to end up with community. Community is the start, the core, and the truest foundation of what we do in public health and health promotion. If we truly want to deal with the injustice of health inequity we need to not just understand and appreciate community concerns. We need to be with the community and speak a language that matters. Or don’t. Perhaps we need to start with deep inner peace, silence, and embrace profound listening. We are in the right country to do this. It’s called Dadirri.






